Last Updated on June 3, 2023
Many patients are told that they have bone spurs in their back or neck and, as a result, that bone spurs cause back pain. However, bone spurs by themselves are only an indicator of spinal degeneration; the presence of bone spurs does not necessarily mean that they are the true cause of back pain.
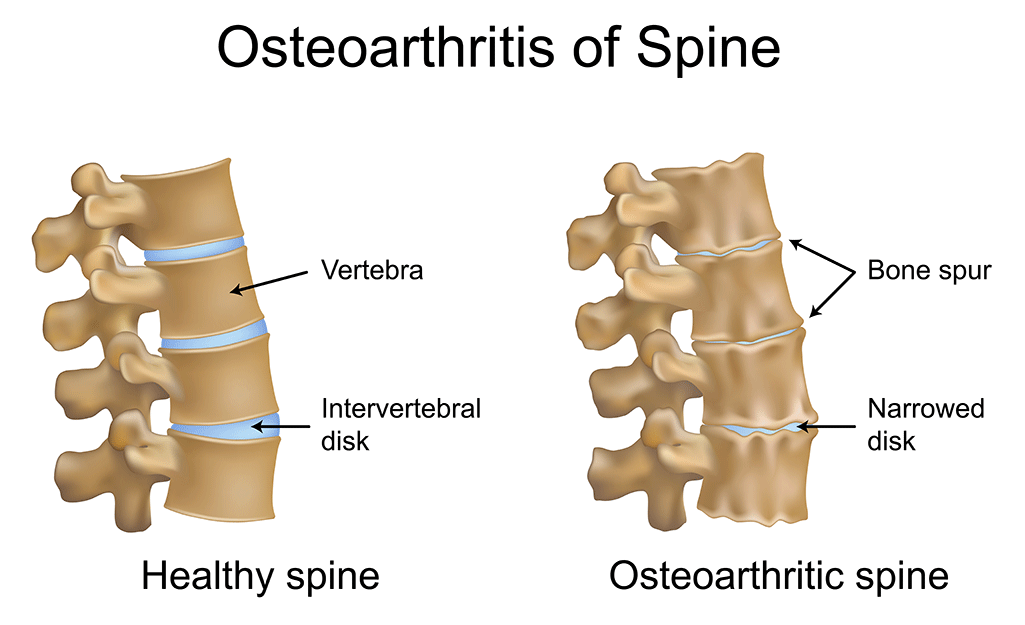
The term “Bone spurs” Is actually a bit of a misnomer, since the word “Spurs” Means that these bony masses poke or pierce some part of the spinal anatomy and cause pain. However, contrary to this belief, bone spurs are actually smooth structures that form over a long period of time. Essentially, osteophytes are a radiographic marker of degeneration (aging) of the spine, which means that they appear on X-rays or MRI scans and are, by and large, a standard finding as we age. Over the age of 60, bone spurs on the spine are quite common.
Bone spurs and the anatomy of the spine
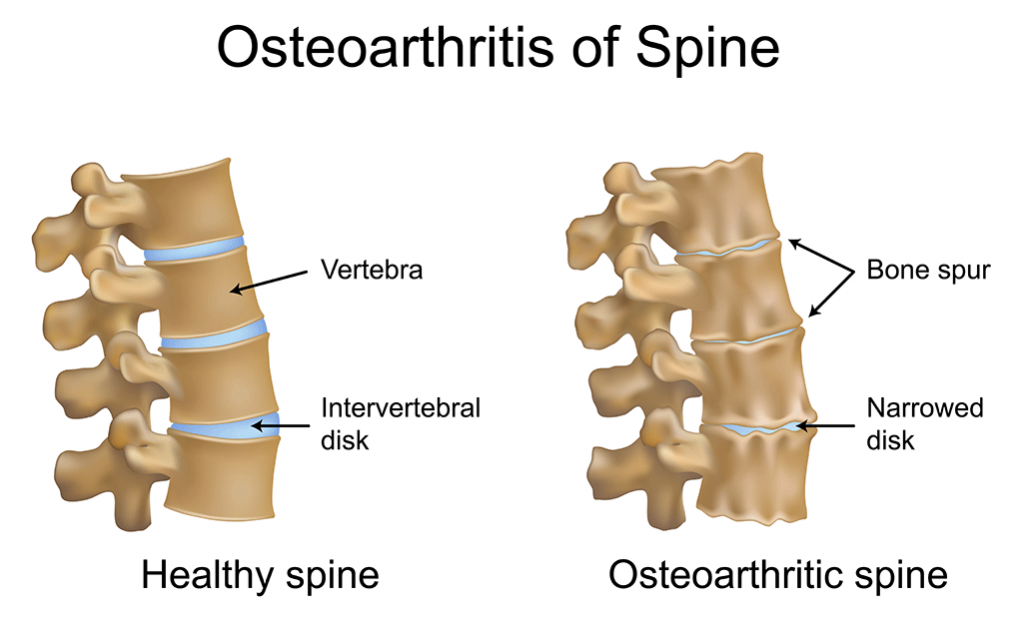
The human back consists of thirty-two separate vertebral segments that are separated by intervertebral discs made up of collagen and ligaments. These discs provide a limited level of flexibility and mobility in each segment of the spine and are shock absorbers. The cumulative effect provides full range of motion around the axis of the spinal column, especially the neck (cervical spine) and lower back (lumbar spine). Movement between each segment is limited by the coarse outer ligaments of the disc, as well as the joints that move (articulate) at each level of the spine (facet joints). Under each joint, just behind the disc, is a pair of nerve roots that exit the spinal canal. The exit wound (foramina) through which the nerve passes (disc in front, joints above and below) is relatively small and has no room for anything but the outgoing nerve. Under the influence of factors such as age, trauma, and poor posture, there is an accumulation of damage in the bones and joints of the back. Ligaments weaken and excessive mobility occurs in the joint as the disc substance gradually wears away As ligaments in the central spinal canal and foramina thicken, compression of the nervous system causes clinical symptoms Degenerative changes in vital tissues, which are standard, begin in early adulthood, but usually this slow procedure is not manifested by nerve thickening until the sixth or seventh decade. Factors that can accelerate the development of bone spurs and degenerative processes in the spine include:
- Congenital or hereditary
- Nutrition
- Lifestyle, including poor posture and poor ergonomics
- Traumatic exposures, especially sports-related injuries and car accidents.
Lifestyle, including poor posture and improper ergonomics injurious injuries, particularly sports-related car accidents and injuries. As always, to prevent or minimize back pain, it is usually highly recommended to maintain good physical fitness (both in terms of aerobics and strength training) and to maintain good posture throughout life. There are several common spinal conditions that are associated with the development of bone spurs, including osteoarthritis and spinal stenosis.
Osteoarthritis
Medical providers often refer to these changes as spinal arthritis or osteoarthritis of the facet joints, and this condition is a standard source of back pain in older patients (over age 55 or 60). Osteoarthritis can cause stiffness and pain in the lower back that goes away after movement, usually getting worse in the early hours and then getting worse again by the end of the day. The most common root cause of cervical and lumbar osteoarthritis is genetic predisposition. Typically, symptoms of osteoarthritis appear in patients between the ages of 40 and 50. Men tend to develop arthritis symptoms at an earlier age, but postmenopausal women, whose spines become stiffer (accelerated bone spur formation), quickly approach men in the prevalence and severity of osteoarthritis.
Spinal stenosis
Bone enlargement leads to spinal stenosis and can sometimes lead to narrowing of the spinal canal. This condition can cause a pinched nerve, resulting in leg pain that does not get better when the patient stands and walks, and does not get worse when they sit. Spinal stenosis cannot be prevented, but it is definitely treatable. Facet joint inflammation often causes back or neck pain and irritates the muscles in the neck and back. Typical symptoms include:
- Blunt pain in the neck or lower back when standing or walking
- Radiated shoulder pain (often accompanied by a headache) in cervical spine lesions (see. Cervical bone spurs)
- Radiating pain in the butt and hip with changes in the lumbar spine.
Signs of bone spurs increase with activity and often improve with rest. Typical lumbar bone spur symptoms often improve when a person leans forward and bends at the waist, such as leaning on a cane or shopping cart. As nerves become compressed, patients with bone spurs experience a number of neurological symptoms, including:
- Pain in one or both arms or legs
- In very rare cases, bowel and bladder incontinence may occur.
Medical conditions other than bone spurs, including but not limited to diabetes, poor blood flow to the arms and legs, spinal tumors, fractures and spinal diseases, can also cause the symptoms described above. Many of the symptoms of bone spurs resemble generalized rheumatism, arthritis, back strain and muscle fatigue, and acute disc tears with nerve compression. Because the typical symptoms of bone spurs are in many cases similar to a number of other possible conditions, it is important for the patient to consult with appropriate medical professionals for a thorough and accurate examination. Diagnostic evaluation begins with a clinical examination. The physician should perform a detailed neurological examination and examination of the spine for spinal nerve and spinal cord compression. The key to the diagnostic procedure will be to compare the patient’s history, symptoms, and any additional tests to find out the cause of the patient’s pain. Common diagnostic tests to aid in the investigation include: Electrically conductive tests are usually performed to document the severity and extent of spinal nerve damage. Radiography begins with x-rays of the spinal column to determine the extent of arthritic changes and bone spur formation. If there are negative changes on these scans, the doctor may find or prescribe additional radiographs. Computed tomography (CT) scans with myelography and/or MRI can provide detailed information about changes in the architecture of the spine and the degree of nerve compression. With these scans, the doctor will correlate clinical symptoms with the x-ray findings and recommend a correction strategy, with regular consultations with the spine surgeon. As noted earlier, a person may have bone spurs present in the above images, but bone spurs may not be the cause of the patient’s pain. As a result, while a scan is a useful tool in the diagnostic process, it does not, by itself, make a diagnosis. There is a wide range of treatment options available for symptomatic bone spurs in the back.
Non-surgical treatment for bone spurs
Most patients with mild to moderate nerve compression and bone spur irritation can effectively manage their symptoms with non-surgical back treatments, among others:
Medications
Medications, including anti-inflammatory drugs and muscle relaxing pain relievers, for about 4-6 weeks.
Short rest intervals
Activity can cause inflammation in the joints, so short rest intervals are necessary first.
Rehabilitation treatment
After 1-2 weeks, physical therapy, exercise and chiropractic care often relieve painful joint conditions. By improving posture and back, these techniques attempt to restore flexibility and strength to the neck and possibly reduce nerve compression. However, for irradiating pain in the leg and arm, nerve compression should be investigated before any type of rehabilitation therapy.
Injections
Repeat injections may be indicated, although the effects are often only temporary. Pain relief after an injection may allow the patient to continue rehabilitation. If these non-surgical measures to treat bone spurs are ignored, consultation with a back specialist is necessary. If patients suffer from acute pain, early referral to a specialist or if there are clinical signs of compression and nerve damage is advisable.
Back surgery for bone spurs
Surgery, such as a laminectomy, is designed to relieve pain and neurological symptoms by removing bone spurs and thickened ligaments that cause nerve compression, which have been painful. Many patients who have undergone bone spur surgery have good results, often getting relief for years and an improved quality of life. Studies have shown that age is not a leading factor in determining whether a person will benefit from back bone spur surgery. However, medical conditions often associated with age, such as heart disease, diabetes, and high blood pressure, can affect the risk of surgery and therefore should be considered when choosing surgery. If nerve or spinal cord compression causes persistent pain or loss of motor activity is documented on examination, spine surgery to remove bone spurs becomes necessary. It is important to discuss the risks and benefits of various back surgery tactics with your surgical consultant to understand all potential factors as they relate to the individual patient’s situation.